Which Blood Type May Be Transfused to an Ab Positive Baby Who Has Hdn Caused by Anti-d?
What is Hemolytic Illness of the Newborn (HDN)?
Hemolytic Illness of the Newborn (HDN) is as well known past other names, including alloimmunization, isoimmunization, blood incompatibility, or claret sensitization. It tin range from very balmy, with minimal to no fetal furnishings, to very severe requiring fetal therapy. Anybody has unique proteins (antigens) on the surface of their red blood cells. When our bodies are exposed to red blood cells that do not lucifer our own, the allowed system produces additional proteins (antibodies) that will marking those foreign red blood cells for destruction. There are 2 ways to exist exposed to claret that does non friction match our own: pregnancy or a blood transfusion. Once antibodies have been fabricated, they are present for the rest of our life.
If a adult female has made antibodies, either as a result of a prior pregnancy or blood transfusion, and she becomes pregnant, those antibodies can cross the placenta. If the fetus carries red blood prison cell proteins that are not compatible with maternal blood, the maternal antibodies may cause devastation of the fetal red claret cells. If enough fetal red blood cells are destroyed, fetal anemia will occur. Since HDN usually occurs during pregnancy, and less commonly through a claret transfusion, this rarely causes fetal anemia in a first pregnancy. Withal, once it appears, it tends to become more severe with each subsequent afflicted pregnancy.
Hemolytic Disease of the Newborn (HDN) Diagram
The nearly common red blood cell incompatibility is due to the Rh poly peptide (also called D protein). Rh disease is the only incompatibility that can be prevented through administration of a special treatment chosen "immune globulin" during times of potential exposure to prevent antibody formation. It is recommended that all Rh-negative women receive Rho(D) allowed globulin during pregnancy and after delivery if at that place is a possibility that the father of the baby carries the Rh protein (is Rh positive). Other proteins that can cause HDN include Kell, Duffy, and Kidd, along with many others. These less common causes cannot exist prevented with immune globulin.
How practise I know if I have HDN?
It is routine to obtain a blood test chosen Type and Screen on every significant woman at the starting time of her pregnancy. This identifies your blood blazon and checks for the presence of maternal antibodies that could cantankerous the placenta and affect the fetus. If antibodies are present (a "positive" antibody screen), further studies are needed to check the amount and type of antibodies present. The level of the antibodies is chosen a titer. When the titer reaches a level that could cause fetal anemia, it is called a critical titer. With the exception of Kell antibodies, we would not expect fetal anemia to occur without a critical titer.
What will happen during pregnancy?
When a pregnant patient has a positive antibody screen, information technology is important to determine if the fetal blood type is incompatible with maternal blood type. In some cases, testing the father's blood will answer this question. For some of the incompatibilities, fetal blood type can be adamant by drawing maternal blood. Other times, an amniocentesis (removal of amniotic fluid from the uterus through a needle procedure) may exist required to determine if fetal claret is compatible with maternal blood. Once we determine if in that location is an incompatibility betwixt the female parent'southward claret type and the fetus's blood blazon (or if we are not sure), we follow the titers by testing maternal blood regularly throughout the pregnancy. If a critical titer is reached or if the antibody is to Kell antigens, the pregnancy is followed with weekly ultrasounds. Although some pregnancies volition demand weekly ultrasounds early in pregnancy, in most pregnancies this starts in the belatedly 2d or early third trimesters.
At the time of ultrasounds, the blood menses to the fetal encephalon is measured through the acme systolic velocity (PSV) of the heart cerebral artery (MCA). Fetuses with anemia increase the menstruum of blood to the fetal brain. A specific ultrasound measurement of this blood menstruation correlates with the likelihood of fetal anemia and can determine the need for a fetal blood transfusion. When fetal anemia is very severe, it can lead to a condition called hydrops when swelling or excessive fluid tin accrue in the trunk. This fluid can be seen in the breast, abdomen, or peel. If untreated, hydrops can lead to stillbirth. The goal of intensive claret and ultrasound screening is to enable intervention for anemia before progression to hydrops.
What happens if there is fetal anemia?
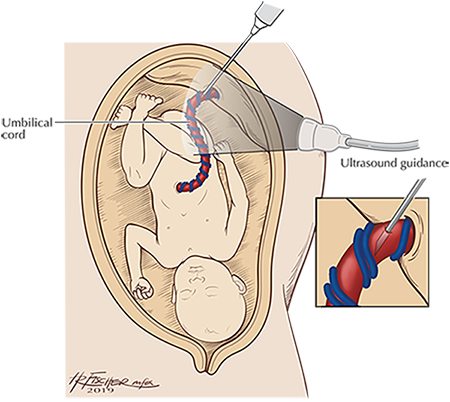
If fetal anemia is suspected, we recommend sampling the baby's blood through a procedure called cordocentesis. The cordocentesis is washed under ultrasound guidance. A needle is placed into the fetal umbilical cord to sample the fetal blood, mensurate the blood count, and perform a blood transfusion if needed. Many fetuses will need more than one transfusion before the pregnancy is delivered.
Cordocentesis and Intrauterine Fetal Transfusion Diagram
What to await at birth?
Fetuses that crave transfusions within the uterus usually deliver between 34 and 37 weeks' gestational age. Virtually half of these newborns volition require a transfusion after birth, and almost all will require handling for jaundice (when skin, and possibly the white of eyes, plough a yellowish color due to buildup of bilirubin), usually with phototherapy (exposure to fluorescent lite bulbs or other sources of light). The newborn will often demand to exist in the hospital longer than the mother. Some babies may be four-6 months old earlier they completely recover the ability to make their own carmine blood cells, so they must exist closely followed by an experienced pediatrician.
Make an appointment
For more data or to schedule an engagement, phone call 734-763-4264.
Source: https://www.mottchildren.org/conditions-treatments/peds-fetal-medicine/hemolytic-disease-of-the-newborn-or-alloimmunization
0 Response to "Which Blood Type May Be Transfused to an Ab Positive Baby Who Has Hdn Caused by Anti-d?"
Post a Comment